Ollier Disease is a nonhereditary condition in which the patient develops multiple benign cartilage tumors, or enchondromas. While isolated enchondromas are not terribly uncommon, Ollier Disease (or multiple tumors) is quite rare. It has been estimated to occur in less than 1 in 100,000 births. It is believed to be non- herditary and related to a spontaneous mutation. The basic underlying issue in Ollier Disease, the multiple benign cartilage tumors, does not seem terribly concerning. However, there are two reasons why this can be a very difficult condition.
First, and most concerning, there is a “high” risk of malignancy. Some estimate this to be as high as 25% of patients. Either the previously discussed benign cartilaginous tumor can become malignant or another tumor may present. This can include scary things like chondrosarcoma (malignant cartilage tumors) or even brain tumors. For this reason, patients with Ollier Disease are monitored closely over time.
Ollier Disease is different than Maffucci syndrome which is a related condition in which patients have enchondromas as well as vascular anomalies, hemangiomas. These are essentially blood vessel masses just below the skin which can lead to skin discoloration.
The second difficult issue is bone dysplasia or bone deformity. The cartilage growths can lead to abnormal growth in any bone affected. This can be most difficult to treat if it affects a segment with two bones such as the forearm (with radius and ulna). In this situation, slower or angled growth of one bone affects the function of the unit. The challenging task is monitoring and then intervening at the appropriate time to minimize such deformity and functional limitations.
Ollier Disease typically presents at a young age but is typically not noted at birth. The enchondromas are painless and it is the deformity or the functional limitations (i.e., a lack of forearm rotation) that lead to presentation to the physician. One side is predominantly affected. As an upper extremity surgeon, I most commonly encounter and treat enchondromas in the hands or forearm bones.
Here are some images from a recent patient with Ollier Disease. The diagnosis may not be straightforward but these x-rays are very helpful.
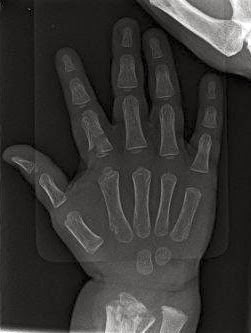 |
| Right hand xray in Ollier Disease. Not the abnormal appearance of the index finger proximal phalanx. |
 |
| Ollier Disease with humerus involvement. |
 |
| Finally, Ollier Disease affecting the radius. This concerns me the most as the growth of the radius is already affected and will only likely get worse. |
What type of monitoring is standard for Ollier? Starting when and how often?
Betsy, thanks for the question. Typically, children (i.e., still growing) are followed at least yearly for a clinical examination and x-rays (maybe every 6 months for a few years and then yearly). Once the child is done growing, follow- up is less frequent and is based on concerns related to a growing mass and pain. Rapid growth with pain is the most concerning signs and likely warrants further workup with possible biopsy. I hope that helps.
Hi Dr. Goldfarb. My daughter was diagnosed with Olliers disease last month. I am devastated as you can imagine. So far all we know is that there are noticeable bumps on her middle finger and ring finger of her left hand. It was diagnosed when we noticed some " swelling " and she told us she hurt her finger at school. They told us she had a fracture on her middle finger and has Olliers disease. We are waiting for a full body MRI that is to be conducted on the 20th of August. Can we hope that this disease is just effecting the hand or is it always throughout the patients body? Information is hard to find and often contradictory. Is she able to have the best care possible here in Pittsburgh, Pa? Any help or info would be greatly appreciated. Thank you.
Hi Olivia,
Thank you for the question and I am sorry to hear about the diagnosis. As you have learned, information is indeed very hard to come by and part of the reason for that is the wide range of presentations between patients. While Olliers may be more common in the longer bones, we do occasionally see it confined to the hand (s). Typically multiple enchondromatosis is on one side of the body but, again, there may be some variability. The bottom line is that you will know more with the MRI and, of course, over time. If I can answer additional questions, please feel free to email at congenitalhand@wudosis.wustl.edu.
Thank you again and good luck.
Hi olivia can you please post the latest heath status of your daughter.? How old is she, does this ollier deasease remain as it is without noticeble growth? Even my daughter had same diagnosis, hence asking. She is 7 years now
Good morning.
My daughter was diagnosed with Oller's on July 31, 2017, just days before her fifth birthday. She has an appointment set up to see you soon. I am curious though, can this have anything to do with her immune system? Meaning weakening it? She has been sick, literally, only once in her life. Now she has classic symptoms of strep throat, which we are seeing the doctor for here in a little bit. Is this possibly from Oller's (not strep, but weakened immune system), or maybe just from attending school in general. I cannot help but wonder. I will have a million other questions when we see you at her appointment, I am just wondering this for now. Thank you so much.
Heather. I am not aware of immune system issues with Ollier's. However, there could be a condition associated with Olliers- just not one I have seen before.