There are multiple websites which detail trigger finger diagnosis and treatment. The AAOS (American Academy of Orthopaedic Surgeons) is a great site and the following link is as good as any.
http://orthoinfo.aaos.org/topic.cfm?topic=a00024
Trigger digits in kids are very different and again, we don’t know why. A couple of thoughts.
1) Most importantly, it is almost always a trigger thumb. Trigger fingers are rare in kids but trigger thumbs are “common,” at least in my world.
2) The term congenital (meaning present at birth) is often used in describing trigger digits/ thumbs in kids. This is not accurate. There are several (at least 3) studies which look at a large number of newborns and trigger thumbs just don’t exist. The appear later. So the best term is pediatric trigger thumb.
3) Kids almost always present with the thumb in a bent or flexed position at the distal joint- the IP joint. Typically it is stuck in that position. Occasionally, kids can straighten the thumb but usually it is just stuck.
4) It doesn’t hurt. Because it is stuck, there is no pain.
5) Function is usually pretty good but we worry about function over time- in school with writing and scissorts, etc.
For those who see kids with trigger thumbs or fingers, the diagnosis is clear. The thumb is stuck in a bent position and sometimes there is swelling at the base of the thumb (MCP joint). We call this a “Notta’s node” and it is where the tendon gets stuck in the sheath. We don’t need x-rays or MRIs.
Treatment for trigger thumbs or fingers.
There are 3 options for treatment.
1) Ignore it as it might get better. This is not unreasonable given that it doesn’t hurt but in our experience, rarely does this go away on its own. But, a 6- month trial of watchful waiting is certainly a reasonable plan. This is the recommendation from Korea with a good study supporting that it will help. Dr Baek is an extremely well respected surgeon who has written on many topics in kids hand surgeries. In his study, 4 years after the first visit, about 60% of kids had resolved and another 20% were improved. http://www.ncbi.nlm.nih.gov/pubmed/18451388 These are impressive numbers but obviously require some patience from the patient, family, and surgeon.
2) Stretch and splint. There is little data to support splinting of the thumb but there is actually good data to support considering a splint and/ or stretching for trigger finger. http://www.ncbi.nlm.nih.gov/pubmed/22624785
3) Surgery. Surgery works for pediatric trigger thumb. It is a small surgery, it is outpatient and takes less than 10 minutes. Patients have little pain after and most heal uneventfully with a cure. Complications are rare and include a risk of infection (likely around 1/200) and scarring. It does require a general anesthetic but again, minimal risks. Trigger finger surgery may be more complicated as it can require a more extensive operation compared to trigger thumb. It is just less predictable. Still effective and reliable.
The decision of when to go to surgery is not easy. It depends on the family perspective, the time that the trigger finger has been present, and the surgeon’s beliefs. For me, a conversation between the family and myself helps to bring all the issues out and guide the decision. In the USA, we tend to be more aggressive than our Asian counterparts about the decision of when to go to surgery.
This is a case of a pediatric trigger finger. Again, much less common than trigger thumbs. This case had a swelling or “Notta’s node” at the A1 pulley which limited extension. At surgery, the A1 pulley was released and the finger extended. Additional surgical dissection was not required and the patient’s condition resolved.
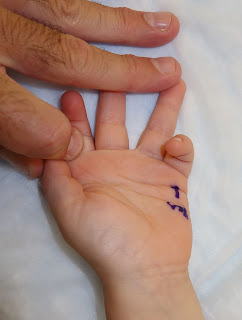 |
| Pediatric trigger finger which is more rare than trigger thumb. Not the flexed position of the finger. It could not be straightened. |
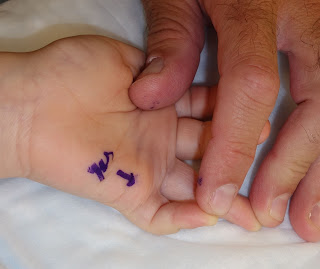 |
| I am trying to straighten the finger but it is blocked in this pediatric trigger finger. |
 |
| Bilateral trigger thumb. Photos courtesy of my partner, Dr Wall. |
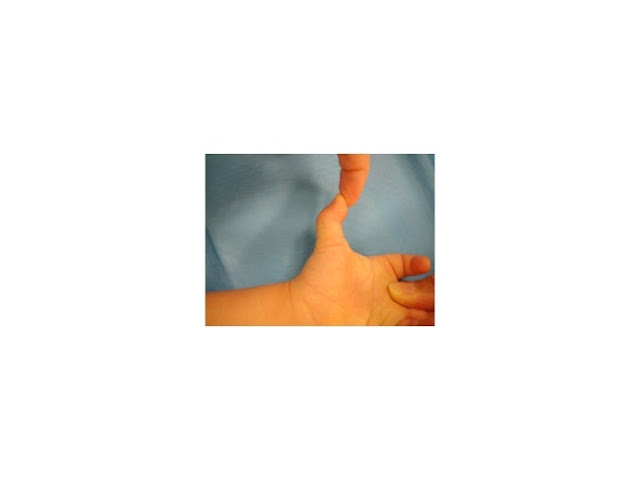 |
| Trigger thumb. We are trying to straighten the thumb but it is locked. Photo courtesy of Dr Wall. |
it does hurt in your little finger as i am 13 and i was born with trigger finger in both of my little fingers and when i was younger it killed and it still does when it gets stuck!!!
Thanks Maddie. For most kids, the thumb or finger is just stuck. When the finger (or thumb) bends and straightens and occasionally gets stuck, that is more like the adult version- I bet it does hurt!
My daughter (3 years old) has this in her left ring finger. It comes and goes – seemingly resolving itself temporarily. Is it possible this is a good sign the trigger finger will resolve on its own? I'm hesitant to take her in for surgery if there's a chance it will. What are your thoughts?
Denise,
Thank you for the question. Trigger fingers are much less common than trigger thumbs in children. They also tend to present like your daughter, with intermittent catching. There is a chance that this could resolve on its own. Additionally, splinting the finger straight at night has been shown to help that potential. Ultimately, if it does not improve, surgery is a reliable option with a hand surgeon who regularly treats children. Good luck.
My son was born with a trigger middle finger. He was born with VACTRAL syndrome as well so I do believe it's related to that but I'm curious 1/ ? are born with trigger fingers. Do you know this information?
Rick and Aubrey, thank you for the question. We do not believe that kids are born with trigger thumbs or fingers. The best research has been done on trigger thumbs but there is a similar belief about trigger fingers. I do not know of any relationship between VACTRL and trigger digits. However, I suspect that the real issue may be camptodactyly (see several blog posts on the topic) as this can happen from birth and is often associated with radial deficiency (a part of VACTRL). Camptodactyly may be treated with stretching and splinting or, on occasion, with surgery. Good luck.
Hello… I am looking forward for Trigger Finger Treatment In Phoenix… for which I have been research since month… Thanks for this …
I am glad the post was helpful. Good luck Melissa.
My daughter was born with all ten triggered. At four years old she had two surgeries to release all ten.
Karen,
Thank you for your comment. Triggering of all ten digits is very uncommon and makes me concerned that there might be other medical considerations. Any condition which increases the size of the tendons (whether that is by increased actual tendon size or connective tissue around the tendons) can cause triggering. Mucopolysaccharidosis is one such example. Good luck.
My three year old son started having triggering in his left ring finger in January (age 2y8m at the time). I try to observe his hands at least twice a day – after he has fallen asleep and first thing in the morning. Since January, we have see triggering occur in 4 additional fingers and one thumb. It seems transient – a finger will trigger repeatedly for a period of days or weeks, then stop or occur only very rarely. Right now we are seeing it mostly in his two ring fingers.
I should note that he has very short fingers and x-ray shows bone abnormalities (thickened trabeculae with cone epiphyses)
Is this situation common for pediatric trigger finger? How long is a reasonable period of time to wait for triggering to resolve on it's own before pursuing surgery? Are there other conditions we should inquire about?
Betsy,
Thank you for your question. First, I should restate that trigger finger is much less common than trigger thumb in children, by a factor of 10 at least. But trigger fingers do certainly occur. However, the situation that you describe is very different. 1) Multiple different digits, intermittent. 2) Short finger and x- ray abnormalities (this is not common but can be suggestive of multiple different conditions).
Putting this together suggests that this is by no means a 'normal' trigger finger and you should be evaluated by a physician with genetics expertise and likely an experienced congenital hand surgeon.
I hope that is helpful. Good luck.
My son is seven months old. His thumb was alright when he was born. But now has a trigger thumb from past a month a two.we are unsure from when it is. We are trying to straighten the thumb, but it is locked. We consulted a physician here in India and he said that surgery is the only option for trigger thumb. What can we do about it? Do we have to wait until he turns 1 year old? Can we do some stretching excercises? Can we try the splint method? If so, how do we do it?As of now we are just massaging.
Your son's story is typical. In addition to Dr Baek's work, mentioned above, other unpublished research from the United States (Dr Hutchinson) supports the concept of watching and waiting. The trigger thumb is unlikely to cause pain or limit function and it may get better over the next 1-2 years. However, surgery can be performed at any point with typically excellent results.
My daughter was just born 4 days ago. I just noticed her thumb on the right hand does not bend and her wrist pops when she moves it. I gently tried to bend it and just doesn't. I have been researching online about what it could be and everything that comes up has to do with trigger thumb. Is this something different or the same as trigger thumb?
Thank you for your question Eryca. And congratulations on the birth of your daughter.
While it is impossible for me to know what is going on with your daughter's thumb and wrist, I do have some ideas. First, this does not sound like trigger thumb to me. Trigger thumb does not present at birth. Also, does she have creases at the joints of the thumb? She may have a hypoplastic thumb associated with radial deficiency- see other posts. But, it seems like she should see a doctor who deals children born with birth problems of the arms and hands- typically called congenital hand surgeons.
I hope this helps. Good luck.
My 2 1/2 yr old has trigger thumb. It suddenly locked a couple weeks after his second birthday and we saw a doctor who only recommended surgery about a month later. We've opted to not do surgery at this point and have just watched it. Occasionally I'll sit with him and apply gentle pressure to the bend until it straightens (takes about 5-10 minutes depending on how still he sits). He's not in pain and has just adjusted to it in his life. I'd really like to try splinting it to see if it helps further. Do you know how we can get one?
Tracy, thank you for your question. As mentioned in my post, the role of surgery or the timing of surgery are in question. In my view, there is no harm in watching and waiting at least for awhile. There is some concern that after a few years, there can be compensation with extra extension at the MCP joint. Surgery is an "easy solution" with really good results (although no matter how simple there is a slight risk of complications).
Stretching is certainly appropriate. Splints have not been proven effective and it can be very difficult to convince a child to wear it. But any hand therapist can help.
Good luck.
i am an 18 year old girl i had trigger thumb since i was 4 it hurts me when i am writing or holding anything i have read that i have a 50 per cent chance of developing a permanent flexion contracture so does it mean that my thumb wont be normal again even if i had the surgery?my parents are afraid about me having the surgery cus they think we had a bad doctors in egypt
Esraa,
Thank you for the comment. Your story is unusual- that is – to have had a trigger thumb for so long. You need to make sure this is the correct diagnosis. But if it is painful, surgery makes sense. If your thumb has been stuck in flexion for 14 years, you are correct, it might not straighten out even with surgery. However, there is still a chance that surgery will help with both motion and pain.
While I cannot speak for all the doctors in Egypt, there are certainly good ones. And, this surgery is usually successful.
Good luck.
My son who is now 20 years old is unable to bend his thumbs. He was born this way. He had surgery on his left thumb when he was around 9 years old. He had no tendon in there. He was sent to Shriners by the doctor to see if he needed genetic testing done for other abnormalities. Doctors there said it wasn't necessary. My question is what causes this? Are there other issues he should be aware of? Thank you!
Pam, thank you for your question.
While trigger thumb can cause a stiff thumb, there are other explanations as well (perhaps I will expand this for a future post). In my experience, the most common other cause is a small thumb with tendon interconnections that limit motion (pollex abductus). But there are also stiff joints (symphalangism) and other causes. Without a clear diagnosis, I cannot offer a list of associated conditions although I agree, this is an important concept. While it may be past the point of surgical intervention, a visit to a congenital hand surgeon may offer you and your son important information on causes, associations, etc.
Our daughter is 6 months old and just developed a trigger thumb. Should we be straightening her thumb every time we see it is stuck? (It does seem a little uncomfortable for her each time it pops back and forth) Or should we literally just watch it over the next several years.
Williams,
Thank you for the question. We typically do not recommend straightening it when it is stuck because, as you note, it is typically at least a little bit painful. Most kids have trigger thumbs that are stuck in the flexed position. In those situations, gentle stretching might be helpful because, as noted above, it might get somewhat better over time. Especially in a 6- month old, watching and waiting makes sense. Good luck.
My son is 18 months and we just noticed he has bilateral trigger thumb. I'm inclined to believe he was born this way and grew into the condition. I say this because his brother, my step son had the same thing. He had the surgery at 2 1/2 and his thumbs are perfect now. There has to be a genetic component? I just pray my little guy has a successful surgery like his big brother.
Hello worried momma,
First, as you can see from the posts and comments, your son will do great. And, as your step son demonstrates, most kids do wonderfully if surgery is done. It is one of the most successful surgeries we offer.
And I agree that there may be a genetic component. But while we do sometimes see this is siblings, most of the time we do not.
Good luck.
Hi. I'm sixteen years old and I've also had trigger thumb since I was four. It's always slightly bent and whenever I straighten it, it hurts. The longer it's at rest, the more it hurts when I try to move it. When I was a kid, I thought it was just another injury that would go away. I've had it for so long that I never even remember to ask the doctor about it. I guess I'll have to go through release surgery.
Hello Cameron M. and thank you for your comment.
Your story is not typical in that you have dealt with this for many years. A hand surgeon will have to examine you to confirm that you do have trigger thumb. If truly not a big deal, then I would avoid surgery. But, if this is painful on a daily basis and you are found to have trigger thumb, surgery might be a pretty straightforward solution. Good luck.
We just noticed that our 2 year olds thumb locks. Sometimes he cries but other times he just uses his left hand.no have been able to straighten his thumb but it cracks loudly. He laughs when this happens but it scares me. Is there danger in me straightening his thumb?
Thanks for the question. It does seem likely that this is a trigger thumb. In most kids, the thumb is locked in a bent (flexed) position but in some kids the thumb will pop into a straight (Extended) posture. Most kids do not seem to have pain but occasionally, as you experience, it might hurt.
Good luck.
Hi! I am a 26 yr old female who has a question. My parents say that I was born with congenital trigger thumb in both hands, so I am unsure when it developed. I do know that I had surgery on my left thumb around my 6 month old mark ( I still have the scar on my thumb) but for some reason they never did the surgery on my right hand. As I grew, my right thumb would constantly lock and I would physically have to straighten it out with my other hand (it would unlock with a very loud pop and pain). As I became older, my right thumb slowly ceased to lock. I'm not sure when this started to happen, but by highschool it wasn't locking up anymore. However, I find that as an adult, when I bend my right thumb I can feel a slight 'catch' and if I listen closely, especially by my ear, I can hear a tiny pop. My thumb will ache if I bend it too often, so understandably, any sort of repetitive motion with it will cause it to ache (specifically in the joint). Do you outgrow childhood trigger thumb? Or is it possible for it to linger after you've grown? (I'm not sure if this is relavent or related at all but I have very tiny hands. Almost everyone I meet over the age of 8 had bigger hands than me…)
Kayla,
Thanks for sharing your story. While the majority of doctors favor surgery as a straightforward way to treat trigger thumb in kids, there has been a trend to try and avoid surgery. This is because of an excellent long term study on kids in Korea who did seem to get better over time (with a nearly straight thumb). But many of those kids did not fully recovered and many did not have the same motion as the other side.
So, while many kids improve over time, not everyone completely "grows out of" their trigger thumb. Your situation seems to be that of a general improvement but incomplete resolution. Clearly, if this is just a nuisance, watching and waiting might make sense. But if more, a visit to a hand surgeon who treats both kids and adults might make sense.
Hi,
My 3 n half year old daughter was born with congenital curve pinky finger, her finger is so small that splint doesn't stay on it for long. Could you please suggest what can we do as hand surgeons doesn't want to do surgery at this point of time and want to see the outcome of splint. Any good design of splint which are used in this kind of case?
Your recommendation would be appreciated.
thanks
Hello,
Thanks for writing. What kind of bend does your daughter have? Is the finger bent towards the palm (camptodactyly) or towards the ring finger (clinodactyly)? Sometimes early surgery makes sense but we usually do often try a splint first. In young kids, the splint often needs to be included in the splint.
Hi thanks for this site..It really helped me to understand more about this issue..And the pictures are awesome…My 3year old was born with this…
Concerned,
Thank you very much. I am my site is helpful. Good luck!
Dr. Goldfarb,
Thank you for your reply. I just wanted to share that my son has since been diagnosed with Acrodysostosis Type 2. The trigger finger and thumbs still occur on occasion, though much less frequently. We had splits made which I put on him at night when we see repeated triggering. The doctors we've seen speculate that triggering will always occur as a function of his hand deformities.
Betsy,
Thank you for the followup. I am glad the splints seem to help. Good luck!
Hello! Thanks for the site. Great information. Our 4 yr old has a trigger thumb (stuck in position) on one hand, and triggering pointer fingers on both hands, which he can flex and trigger. He can usually un-pop them, but sometimes needs help to straighten. We tried splinting for a month at night, and full-time for a few weeks, but didn't see any improvement. We're in the midst of a 6 month wait-and-see period. We see him using his thumb and middle finger or middle finger and palm to pinch and manipulate things rather than using his pointer fingers, and he tends not to grasp things with a firm hand, but with a floppy fingered hold. Wondering if you would recommend pushing for more hand therapy work, surgery or rest and see? Thanks, Christy
Christy,
Thanks for the question. Your son's multiple trigger digits is really unusual. Trigger thumbs are far and away the most common digit affected but there are occasional trigger fingers. Bilateral index finger trigger fingers are really quite rare and sometimes can be associated with other conditions. If the splints have failed, in my opinion, it is reasonable to consider proceeding with surgery. I sometimes use the 6- month waiting period but typically with trigger thumbs. I don't think additional therapy is likely to help.
Good luck,
I started to notice my daughter tumb bends she cant put it back up we might think she might have trigger finger we dont even know how long this was going on she doesnt tell me it hurt and it only her right hand tumb am scared to know what going happen when she get older
Sahra,
It does seem like your daughter has trigger thumb. In most kids, the thumb is stuck in a bent position but in others, the thumb can get stuck at different times. This may continue but there is a chance she could grow out of it. If this becomes bothersome or more frequent, the simple surgery can be curative.
Hello Doctor,
2 days back first time my 2 yr old son's left thumb got stuck in a bend position. it happened few times a day but otherwise normal. everyday, it is happening 3/4 times a day with no pain. When I am straightening his finger a pop sound is coming and it is getting straight. whenever it is happening, it is 4/5 times and then whole day he is fine with no symptoms of trigger thumb. Can you please suggest what i should do?
Regards,
Alaknanda Sen
Hi sir, my daughter is 19 months and found she had a bent on her left thumb and a lump bone at the thumb base. Is this a trigger thumb? I am so worried. Should we watch massage and wait to see? If yes till what age? Or should she get a surgery instead? Thank you.
Alaknanda,
Thank you for sharing. Your description sure does seem to be of an early trigger thumb (one that is not stuck in flexion). I would recommend an evaluation by a hand surgeon who specializes in children. Sometimes, at an early stage like this, night splinting can be considered. Good luck.
Kanha,
Thank you for writing. It is likely that your daughter has a trigger thumb (but obviously, there is no way for me to know for certain). As long as that is the correct diagnosis, there is no harm in watchful waiting but I would take your daughter to be evaluated by a hand surgeon who specializes in children. Good luck.
I had bilateral trigger thumbs as a child. I vividly remember hitting my thumbs on something and popping them "out of place" or straight. It hurt! I had to hold my thumbs down for them to return to where I could actually use them. Eventually they worked themselves out. My son is two and now has one trigger thumb. I'm positive it is because he held his themes as an infant (which is what I did). Now it is stuck. I'm not sure what to do for him. I hate for him to have to deal with the popping out of place… And I'd hate to wait it out and it not resolve over time.
Tiffany,
Thank you for the comment and sharing your experience. As I have shared, most kids have a thumb stuck in a bent position rather than popping in and out of place. Watching your son for a bit certainly makes sense and then you can make a decision on whether surgery makes sense.
Good luck.
Hi Doc,
My Daughter is 3.6 years old now, she has trigger thumbs in both hands.
Now we have started some massage,should we wait and watch?
or we should go for surgery?
thanks in advance.
Alok Singhal
Alok,
Thank you for the question. The decision on whether to watch and wait or have surgery is a family choice together with the surgeon. The benefits of surgery include its reliability (it works) and its simplicity. The risks low. However, the literature has shown most kids improve (although may not become 'normal') over time.
Good luck!
Hello, my daughter is 19 months old and has been diagnosed with trigger thumb in her right hand. There is a nodule at the base of her thumb and her thumb is locked in a partially bent position.I tried gentle flexing but cannot seem to be able to straighten it. Does it take some time for the flexing or stretching to work? As I read other people mentioning that it usually takes them 5-10 mins to unlock their child's thumb, am I doing something wrong? Is there any stretching/massaging guides that you can point me to. Also how long should I wait and see?
Shall really appreciate your help on this.
Thank you
Thank you for the question. Based on your description, I agree that she likely has a trigger thumb. She is certainly in the age range when we make this diagnosis. In most kids, the thumb is simply stuck as the 'nodule' cannot pass through the sheath (a mechanical block). So stretching is not going to work today or tomorrow but there is some evidence that over time, the position of flexion improves (i.e., the thumb gets straighter). Personally, I give families information on gentle stretching but I do not recommend focusing on it- this is a slow process, can take literally years. If there is no improvement over 6,12, or 18 months (family preference), many consider surgery which I believe is very reasonable. I hope that helps. Good luck.
Thank You Dr. Goldfarb. I have consulted a few local physicians but none of them have been as insightful as you. I had just one more question:
I had success straightening my daughter's thumb with some more pressure but it hurts her and goes back to the bent position soon after. I convinced our doctor to try splinting for 3 months and he drew us a diagram for a splint to be worn at night. But I am not very confident on going ahead yet.
At this point, would night splinting be helpful? Can splinting make the her condition worse in any way?
Once again thank you so much.
Night splinting has been proven successful in trigger finger, but not trigger thumb. Most of us who treat kids like your daughter do not recommend splinting. It is unlikely to hurt, but we are doubtful it will help. Time is likely your best "ally" and maybe gentle stretching. The studies that show improvement followed kids over years. I hope that is helpful.
Thank You for all your guidance and support.It's been very helpful
Hello! My daughter was initially diagnosed with a trigger thumb a year ago. We initially thought it may have been an injury because she was 2.5 years old and I was certain I would have noticed it before. As I looked back in pictures though I couldn't find one of her thumb straight past 6 months old. So her thumb was splinted for a couple of weeks and ever since it has been stuck in the straight position. Occasionally it pops back bent but we just pop it back straight for her. I'm very leery of general anaesthetic, any recommendations? Are there any risks associated with leaving it and not having surgery?
Thank you!!
Jacqueline,
Thank you for the question. This is a relatively common scenario (at least in my world). I agree with observation/ nonoperative care to start. Splints have not been shown to help. There are some studies that show the thumbs tend to get straighter and 'resolve' over time. However, there have not been studies looking at what happens when thumbs are straight and don't bend. While this is a decision for you and your doctor, I would consider surgery to improve flexion of the thumb and, I believe, function. Risks are very, very low for this quick surgery. Good luck.
Hi,
I am 24 years old and currently living with bilateral trigger thumbs. I have always thought it was something I was born with and didn't ever look into it. My parents tell me they noticed it when I was about 4-5 years old. My thumbs I noticed are worse in the morning (more flexed) and improve throughout the day. Other than never being able to give a thumbs up, they have not bothered me. When I try to straighten them out, I can pop them so they fully extend but it is painful. I am unable to bend my thumbs when I pop them into extension. How likely is it that surgery would be successful at this point in time? Thank you!
Cue,
Thank you for the question. Certainly this is an unusual situation. Based on your description, I do believe surgery has a good chance of helping you regain more normal thumb motion and function.
Good luck.
Hi. Our 3 year old has trigger thumb in the locked position with swelling at the base of the thumb. Surgery has been recommended. Our preference is to wait until she is 4 as we are uneasy with anesthetic at 3. If we wait a further 12 months is there a risk of the thumb being permanently damaged or locked?
Rachel,
Thank you for the question. Two comments. First, a recent study did not show notable findings based on age at surgery. There is unlikely to be any difference between a brief surgery at age 3 vs age 4. But, on the other hand, your 3 year old will likely be fine no matter when the surgery might take place. Some may argue that earlier surgery may allow more rapid incorporation into use. But no difference in permance or locked status. Bottom line, probably not a huge difference no matter how you consider it.
Hi. My daughter just had a surgery for her trigger thumb. It is been 3 weeks now but the thumb is still not straight. Do we have to wait couple of more weeks to be straight? Thank you
Omar, thank you for the question. Usually motion returns right after surgery but on some occasions, therapy or time may be required. Best to ask your hand surgeon. Good luck.
Hello! My daughter has trigger in both middle and ring fingers of both her hands, by birth. She is 4.5 years old now. I heard that surgery in childhood can result in correction of trigger but the growth of the fingers might be affected and those fingers wont grow to the normal size. Is it so? What is the right age to get surgery done? and if we wait till teenage or adult hood, can surgery be performed then successfully? Thanks!
Thank you for your question. First, triggering of middle and ring fingers in both hands is quite uncommon at 4-5 years old. Confirming the diagnosis will be important. Trigger release surgery does not affect finger growth. If the fingers are catching and there are functional limitations with pain, treatment of some sort makes sense. There is some support for splinting an trigger finger in a child but I am less certain that splinting will be helpful with 4 fingers affected. Nonetheless, it is easy to try a night splint. Or surgery is a reasonable option. Good luck.
My son developed trigger finger on pointer finger (right hand) around 8 months. We were told to wait and see if it self-corrects. He is 13 months now and it hasn't corrected. Recently I noticed his other 3 fingers are curving in like trigger finger. He can release them if he catches them on a toy and pulls, but they mainly stay inwards. Is this common? To go from one to several trigger fingers? We are concerned. Are there splints available for such small hands. And are they effective?
Crystal,
Thank you for the question. First, most kids only have a single finger but there can be multiple although only rarely have I seen them present at different times. Second, and not for conversation on this post, general health issues can play a role (if any). And third, as noted in the blog, splinting can absolutely work for trigger finger (more so than splints work for trigger thumb). But sometimes surgery is necessary (and it is effective). I do not typically just watch and wait. Good luck.
I am13. And i have it in my right thumb i have had it since i was 1 month-old
Thank you for replying. I would hope and believe that you are functioning quite well. Does the deformity bother you or are there certain tasks that are difficult?
Hi. I'm 43 y/o and experiencing trigger finger (ring finger) since January this year and my first time to have this. Every morning my finger locked and I need to straighten it slowly and too painful, the pain won't go away. Is this due to my work as Library assistant for 5 years now? And does my case called as congenital trigger finger? (FYI: operated carpal tunnel released year 2000 on the same hand)
Your advice will be greatly appreciated.
Thanks.
Aireen,
Thank you for the question. You are describing classic trigger finger. I would not call this congenital- rather just a trigger digit. Any surgeon can help with the diagnosis and treatment (often a steroid injection as the first step). Good luck.
My son is 8 now. I noticed his trigger thumb when he was 2 or 3 (I'd need to check his records) and took him to a bone and joint doctor who said there was a decent chance it could fix itself by age 7. He's had times it was forced straight by something (a rigid goalie glove, for instance), and he says that hurts. Did we wait too long? How likely is surgery to be successful now? Or in the future? Finally, is there still a chance it could correct without surgery?
Hockey Mom 33,
Your initial advice was reasonable but it sounds like it did not resolve. In this case, surgery still makes sense and can still lead to resolution but there can be other factors to consider including joint motion at the MCP joint. Definitely needs the input of experience congenital hand surgeon.
Dr Goldfarb, thank you for this article. My 8 yo daughter seems to have something similar – her right thumb locks but it is at the middle joint (and the thumb then sits very straight in her palm, pointing at the base of the second finger) rather than being bent at the distal joint. Does that still sound like trigger finger?
Lee, thank you for the question. This does not sound like a trigger thumb. It may be related to a tendon issue if it does intermittently straighten. I assume that your daughter's thumb can be straightened or straightens some of the time? Or can she just not straighten it ever? She needs to be examined by an experienced hand surgeon for kids. Let me know if/ how I can help further.
Im a 17 year old girl and both of my middle fingers have been experiencing the trigger finger symptoms for over 5 months at least now. The pain isn't really bad but it's annoying and my left hand middle finger hurts much more than my right hand. I have been cracking my knuckles for most of my life and I do not know what could have caused my trigger finger as I have been searching online and I don't have any of the causes, could cracking my knuckles have been a cause, can it be random? Also, since the pain is not bad on my right hand and on my left hand it only hurts sometimes, should I see a doctor or wait it out more?
Hello. I am sorry you are experiencing trigger finger symptoms. This is not related to 'cracking' your knuckles. Most times, the origin or reason for trigger finger is not known. I always recommend an assessment by a hand surgeon to assure the correct diagnosis and to allow a discussion of the treatment options. Good luck!
My son is now 17 months and still having issues extending his ring (original trigger finger), middle, and pinky fingers on his right (dominant) hand. When he crawls (he still is unable to walk independently), he often keeps those fingers bent. When he tries to grab at stuff, swipe the screen on his toys, or spin the wheels on his hot wheels, he only stretches out his middle finger. He can. However stretch his entire hand out at times (to hold his cup or other item that requires a bigger grasp). I have not seen him use any other finger on his hand independently except for his middle finger. We are trying occupational therapy to encourage him to extend them to grasp, poke, and pick up small items. So far, he is not able. We saw a orthopedic specialist today and we're told there is nothing to worry about as he just seems to prefer to use his middle finger. Can it just be preference if he doesn't extend his fingers individually? He doesn't point and that scares us. His pinky finger is curved on both hands. He has never had X-rays. We wondered if those would reveal any useful insights? We were told not to worry and that we needed no follow up unless his fingers trigger and stay that way. We just don't want to delay an early intervention if it will help.
Crystal,
Thank you for the followup question. The bottom line is that this situation is difficult for me to provide advice. As I mentioned, multiple trigger digits is rare and this may represent another condition. An experienced congenital hand surgeon would likely be able to give you another opinion (if your orthopedic specialist is not that). Sorry I cannot give you more information.
Hi
My son was born with his pinky finger bent down, like shown in your pictures, and will not straighten out. He is now 6 weeks old and theres still no progress with extending his finger. I have been rubbing and pushing lightly on the joint to try to exercise it. Is there a chance this will straighten out over time as he begins to grab things on his own or should we do something else? My other son who will be 3 this year was born with both pinkys pointing inward towards his other fingers. His doctor keeps saying it will straighten out on its own but i still have seen no progress in straightening. What should i do?
Heather,
Thank you for the question. A visit with a hand surgeon with expertise with these issues will be helpful both to confirm the diagnosis and institute treatment- whether stretching or splinting. Surgery could, at some point, make sense. It does not sound as though this is likely to resolve on its own. Your other son may have a clinodactyly. This is also unlikely to improve on its own. I hope this is helpful.
My daughter had surgery for her trigger finger recently & after the cast was removed she has to wear a splint at night, but her pinky doesn't stay in the splint very long because it's so tiny. What should I do about this?
Hello. This is a challenging question for me to help with as I am not sure of your surgeon's thoughts. First, I do not cast after this surgery, or if I do, it is for a very short period of time and just for comfort. Second, the surgery should cure the trigger finger and I am not sure of the point of a night splint (yes, for other diagnoses). Sorry that I cannot offer additional insight.
Hello, my son is 6 weeks old. He was born with middle fingers on both hands bending toward the pinky side at the PIP joint. When he make a fist, the middle finger is tucked under the ring and almost pinky finger. I can help him straighten the fingers but he cannot do it himself. He likes to keep them in a slightly flexed position. He can move the middle fingers but not as much as the other ones. We have an appointment with pediatric ortho in 3.5 weeks. He will be 2 months 1 week old by then. Is this too long to wait and what are the treatment options? Thank you.
VN,
Congrats on the birth of your son. I am not sure what is going on but sounds like a correctable camptodactyly. If so, therapy and splinting might be the best bet. Good luck.
Hello.
My 2 year-old has trigger thumb. The doctor said that he must be operated and requires general anaesthetic. Me and my wife we are not comfortable with general anaesthetic. Can we postpone the surgery till he's five or six years-old in order to perform it with local anaesthetic?
Dark Angel,
Thank you for the question. I would not say that trigger thumb 'must be operated'.
1) If surgery is decided, general anesthesia is recommended. It is incredibly safe. Local is not recommended in younger kids.
2) The decision for surgery is a personal one. This may improve over time and even may resolve (good information in the literature) but may not completely go away. However, most kids function well even with an inability to straighten the thumbs completely. However, many families do want a 'fix' for this and surgery does that in a very straightforward, very safe way. Surgery is <10 minutes on each side and recovery is typically straightforward.
I would say this is a family decision in consultation with the physician. I certainly have families who chose surgery after knowing the facts and others that chose to watch and wait. I hope this is helpful.
Thank you for all your input. I have a 2 yr old son with trigger thumb in both thumbs. I had several questions but after reading all the questions on this thread and your answers. I see my questions have been answered. Thank you for your time. And your patience you have repeated your self over and over. must get frustrating. Anyway we appreciate it thank you 🙂
Glad the blog is helpful. Thank you.
My 5 1/2 year old has been diagnosed with trigger thumb in her non-dominant hand. We are trying to decide whether she should have the surgery. We I understand the potential benefits. Are there any risks to not operating? For example, worsening of the condition, or developing arthritis? Are the surgical success rates better as a child than if we were to wait until she was an adolescent?
JS. The surgical risks are incredibly small. Tiny risk of infection- at our center it is less than 1 in 300 and even if this occurs, oral antibiotics are usually the only treatment. As long as the surgeon is experienced, other complications are even less common. Risks to not operating do exist including a risk that the deformity at both the last joint and then next to last joint may not correct (your child is definitely on the older side for this diagnosis). I hope this helps.
I have a 2 yr old boy that has trigger thumb in both thumbs. I had some questions about the subject but after reading all the questions and answers. I feel alot better. all my questions have already been answered. thank you for this thread and your paitents as many people repetitvly asked the same questions over and over again. we all appretiate you and your educated input.
My six year old has woken twice in the morning complaining that he cannot straighten his fingers and that they are locked in a fist. I am able to help him straighten them without him complaining of but he is then worried they will lock again. When I ask him if it is a particular finger he does state it is the ring finger and while he says it is in both hands one seems to be worse than the other. After a little time he uses his hands fine. Any ideas?
Catherine. Thank you for the question. It is difficult for me to know without an examination. This could indeed be a trigger finger(s) or could be cramping. If an examination by an experience pediatric hand surgeon is not helpful, imaging such as an ultrasound could be. Good luck.
My son was born with cleft feet. When he was 3 months I noticed that he had trigger thumbs. He is now 8 months. He can barely stretch his thumbs. I have talked the doctor and she stated that his orthopedic doctor will have to refer him for genetic testing. I am concerned because when he grasp or grab anything he tries to stretch it but it does not straighten completely. Could think be genetic because his feet and thumbs are inward.
Hello Soccorri. Thank you for the question. I do not know of a link between trigger thumb and cleft feet. I am not sure whether the genetic consultation will be helpful.
Hello my daughter 16 months is already did her surgery last 2 days for her middle trigger finger but I'm not see any difference when I try to open her finger is still trigger did u think the surgery is not work and maybe she need more time to open it
Thank u
Thanks Ahlem. While there is usually immediate improvement, at 2 days after surgery, it may be too early to know if the surgery was successful. But, again, usually, the improvement is immediate. Trigger fingers in kids are much more challenging than trigger thumbs. The surgeon must treat fingers with an algorithm such that if release of the A1 pulley does not solve the issue, further steps are taken. If there is still triggering after a few weeks, additional intervention may be necessary. An experienced pediatric hand surgeon is a great resource. Good luck.
Dr. Goldfarb,
My 4 year old son has a trigger ring finger. We’ve been doing a “wait and see” but lately he has been telling me it hurts. He can pop it out sometimes but other times he has to use his other hand to “fix it.” Would splinting work inthis type of case?
I would absolutely try a night splint. There is some evidence that it can help and certainly does not hurt. If it fails to lead to improvement, find an experienced surgery because there is decision- making required at the time of surgery. Ideally, you find a hand surgeon who focuses on birth differences/ anomalies. Good luck.
Hi doctor we already see the doctor today her surgery not successful he said maybe the problem is the bones she will have an x ray after 6 weeks.do u know anything about bones problem?? Thanks
I am not sure what the bony problem could be although a diagnosis of camptodactyly is possible. Good luck.
Thank you for this post. My son is 8 years old. He has left hand trigger thumb and right hand trigger pinky finger. These are from birth. Do I need to do surgery or it will be corrected automatically?
Mahen,
Thank you for the question. It is rare to have trigger thumb and finger on the same hand. Clearly, your son has done reasonably well at age 8 without surgery. However, I would not expect either condition to notably improve over time. If bothersome, surgery might be helpful. This is certainly something that a pediatric hand surgeon could help to evaluate and consider options. Good luck.
Thanks for continuing to respond to questions! My 2 1/2 year old has been diagnosed with trigger thumb and we have been advised to simply observe until he is 4. Am I right in thinking, from your other comments, that even if his thumb is stuck in permanent flexion for a few months, this isn't going to cause any longterm problems? At what point should we begin to be worried if it continues to be permanently stuck? Thanks!
Leslie,
My experience has been that the thumb will do fine despite being stuck in flexion for a few additional months. While I would not disagree with waiting at least some time, my personal feeling is that if the thumb has not improved after 6 months or so, it likely will not. The literature suggests that most of these locked trigger thumbs do improve at least to some degree but, the the US, many surgeons offer a surgical release if the patient is not improved over time. That is my philosophy as well. Good luck.
Thank you for your advice. Much appreciated! I wish you all the best in your work!
Hi Doctor! My son is almost 4, he was diagnosed with trigger thumb last December. We have tried stretching his thumb and it popped up once but immediately flexed back down. He does have the nodules at the base of his thumb and he says his thumb hurts a lot. We have been advised to have the surgery to correct his trigger thumb. Just worried about the possible complications and wondering if we should wait longer ?
Thank you for the question. While it is possible that the thumb may extend more over time, my honest opinion is that surgery is reasonable. Surgery is very safe and effective. Complications are unlikely.
Good luck.
My son is now 30 months and is still having the similar issues. He is unable to stretch his pointer, ring, and pinky finger out independently. He can outstretch all fingers as a whole (about 75% of the way), but he can not isolate them. The only finger that he can isolate on his right hand is his middle finger. He uses it to point, swipe the screen on his tablet, etc. His pointer finger triggers occasionally. Lately, his thumb on has been triggering a few times a week. It will stay bent anywhere from several minutes to several hours. Sometimes he is able to pop it out on his own, but most often, he uses his other hand to pop it out. He complains that it hurts when it first locks.
We had an appointment with a pediatric orthopedic specialist at Children's when he was 17 months and were told not to worry that he was probably just preferring to use his middle finger to point, etc. He had a few months of occupational therapy around that time, but it did not help. His pediatrician said to wait it out until he is 3 because he likely wouldn't be eligible for any surgical intervention until after then due to his age.
We are concerned about congenital issues because looking back at photographs from his birth on– his right hand has always been clenched. We aren't for sure how to request a congenital hand surgeon appointment as we thought that was who we were seeing at his last appointment, but maybe it was just a general specialist? We are worried how this will affect him in the long run as his right hand is his dominant hand and he struggles with utensils, holding crayons, etc.
Crystal,
Thank you for sharing. I completely agree with your inclination to see a pediatric hand specialist. This does seem to be something that may benefit from treatment, whether therapy or potentially even surgery. Feel free to email with additional questions: congenitalhand@wudosis.wustl.edu
I believe my 5 year old daughter has just recently developed a trigger thumb. The other night she demonstrated to me that she can bend her thumb at the joint and make it stick and then pop it back straight again using her other hand. I thought this was strange but didn't think much of it. The following evening (last night) I noticed her left thumb was not as straight as her right thumb and was slightly bent at the joint. I immediately thought about a child that I worked with a few years ago who presented with a trigger finger. So I began massaging my daughter's thumb to see if I could straighten it out. I finally was able to 'POP' it back straight but it caused her quite a bit of pain. This morning she woke up and again her thumb was slightly bent at the joint, I again had to massage the joint until it was free to "POP" back into a straight position. Whenever she bends her thumb ever so slightly, like to turn up volume on a phone or grasp something, the thumb again locks in a bent position. As long as she catches it right away, she can easily pop her thumb back into a straight position with little discomfort; however, if she goes an extended period of time with the thumb in a locked position, straightening it is very painful for her. She can not tell me how long she has been experiencing it but she says she just figured out her thumb can do this.
I did submit a request to schedule an appointment with her pediatrician to. What might cause a trigger thumb to suddenly appear in a 5 year old and what might the prognosis be?
Wendi,
Thank you for the question. A trigger thumb can appear in any age group. While 5 years of age is a bit older than the age we typically see this issue (2 years, or so), it is not uncommon. And the most common presentation is a thumb stuck in a bent (flexed) position. However, again, this presentation certainly happens. One option might be to splint the thumb in extension (ie, straight) and check to see if this helps. Otherwise, and especially given the pain, surgery could be a reasonable step. Good luck.
My son is 3.5 month old and we just recognized his left ring finger has trigger finger. We checked the previous photos and we found out it just started when he was 1 month old.
I am wondering if finger splint helps? Also is it enough to use finger splint just during night?
Thanks for your help
Shawn,
Congratulations on the birth of your son. The brief answer is yes- splints can absolutely help trigger finger. I would recommend that you see a hand surgeon who treats kids commonly and a hand therapist is likely to be involved as well. Night time only splinting may be effective but there are different considerations.
Good luck.
Thank you for the article. My 2 year old has trigger finger of her left middle finger. It has been happening for about 2 months. I am planning on delaying surgery and trying a splint for a period of time.
I'm just curious if there are any other underlying medical conditions besides MPS which are associated with trigger finger/thumb.
Thank you kindly
MPS is perhaps the most commonly associated condition, you are correct. There are no other particularly common conditions.
Good luck.
My son was born with cleft feet. When he was 3 months I noticed that he had trigger thumbs. He is now 8 months. He can barely stretch his thumbs. I have talked the doctor and she stated that his orthopedic doctor will have to refer him for genetic testing. I am concerned because when he grasp or grab anything he tries to stretch it but it does not straighten completely. Could think be genetic because his feet and thumbs are inward.
Dr. Goldfarb,
First, let me thank you taking the time to offer your advice and expertise free of charge to a bunch of strangers. That speaks to your character and provides an enormous amount of credibility to you and your organization.
My 3 1/2 year old daughter was recently diagnosed with trigger thumb after we recognized it would not extend fully. You can also feel the little nodule at the base of her thumb. We took her to a local children's hospital and they recommended she have surgery, but we were floored with how much it was going to cost ($25k billed, $5k out-of-pocket) for a 10-15 minute procedure.
After doing some online research and reading Dr. Baek's studies, I'm now inclined to wait and see if it resolves by itself over time. Would there be much, if any, risk in waiting until she's 5 or 6 to see if it resolves before having the release surgery? At that age, would she be able to do the surgery under local anesthesia instead of general?
Thanks,
Chuck Dukes
Chuck- thank you for your kind words- it is a labor of love on subjects about which I am passionate. I too am shocked at the expense- impossible to justify! Given that this is a 5 minute surgery and incredibly safe (in the right hands), I really don't understand.
Sorry. Off soapbox. Dr Baek's work is compelling and a friend in Utah has tried a similar approach with also reasonable results. My only concern is that this approach is rarely a "full" correction- of course, if the thumb is nearly straight, is there a problem? Finally, unfortunately, at 5 or 6 years, local only surgery is still not an option. The injection of local is very uncomfortable and poorly tolerated until teenage years (at best). But, certainly no harm in watching and waiting for a year or so. Good luck.
Just stopping by for an update to let you know that our daughter’s trigger thumb has completely resolved around age 5 1/2. We took your advice after reading Dr. Baek’s work, and sure enough one day a few weeks ago we noticed her thumb was at full extension. So glad we didn’t elect to have it surgically repaired right out of the gate. Thousands saved on what would have been an unnecessary surgery!
Thank you for sharing and I am so happy with your outcome. While many patients do not resolve their trigger, it is always great to see when the Nonoperative approach is successful.
Hello! I just wanted to thank you for this blog. My 4 year old had bi-lateral trigger fingers (little fingers). The first ortho specialist we saw had said he was familiar with trigger thumbs in peds but had never seen any other digits in pediatrics, other than in his text book. He said it was a straight forward surgery to correct the issue. Having never operated on this particular condition did not sit well with me, especially after finding your blog and reading that trigger fingers in peds can require a more complex surgery. We decided to take our child for a 2nd opinion to our (somewhat) local Shriners hospital. That surgeon was familiar and knowledgeable on the condition. He did an amazing job on my sons hands and the care my son received from everyone at Shriners was better than we could have ever imagined. He has made a very quick recovery and now has full function of both hands! Thank you!!
Natalie- thank you. You captured my "why" perfectly. I am glad the blog was helpful for your family.
Good day.. My 3 year old son was born with normal fingers then all of a sudden when he was about 1 and half years old we noticed that both his thumbs have been bent and can't straighten it at all so its been like this for a while now
Hello. This is a classic presentation. All seems fine until you notice that the thumbs are stuck in a bent position. Its always tricky to know how long the thumbs have been bent b/c younger kids function just fine.
Hello! Messaging from Australia, Hope all is well for you over there during these chaotic times.
I’m a registered cardiac nurse.
I have 14 month old identical twin girls who have mirror image trigger thumb- both are always locked.
A few questions- is this rare for both to have?
Would this be congenital and or genetic even though there is no substantial evidence or documentation to suggest genetics are to blame nor a definitive reason of the cause?
Any other advice or information would be super appreciated! 🙂 thank you!
Hello Sheridan. That is super interesting. There are a few reports in the literature but it does the issue of a genetic component. There is no science confirming this but it makes sense (maybe a genetic predisposition). Thankfully, your girls will do great! As you can see from the blog, in the US, if the thumbs fail to improve (? 6 months), many will proceed to surgery which is safe and reliable.
Hi Doctor,
My 2 year old son was diagnosed with PTT this year in Jan. The doctor gave instructions to massage and asked us to wait and watch for 6 months. He was not much cooperative for the massage. However, twice during the last 2 months, the thumb became straight for a moment on its own and it would hurt him and he would cry. then in few minutes it goes back to the bent position. But he holds pencil and other stuff using this bent thumb and draws or scribbles normally. We are not sure if waiting will really help. Please suggest.
Hello. There certainly remains a chance that the trigger digit will resolve. However, in the situation when there is pain as you describe, I tend to offer surgery sooner. The bottom line is that the surgery is safe and effective and it makes sense to me.
Hi Doctor, my son is 2 years old. His right hand thumb gets bend (it happens three to four times during the last one month) and after some it becomes normal naturally. Sometimes we help to stretch and it gets normal again. What to do?
Hello Nurul. It does seem like trigger thumb although most 2 year olds present with a thumb locked in a flexed/ bent posture. Time may help this improve. Surgery is also curative and safe. Good luck